Diseases & Conditions
Meniscus Tears
Meniscus tears are among the most common knee injuries. Athletes, particularly those who play contact sports, are at risk for meniscus tears. However, anyone at any age can tear the meniscus. When people talk about torn cartilage in the knee, they are usually referring to a torn meniscus.
Anatomy
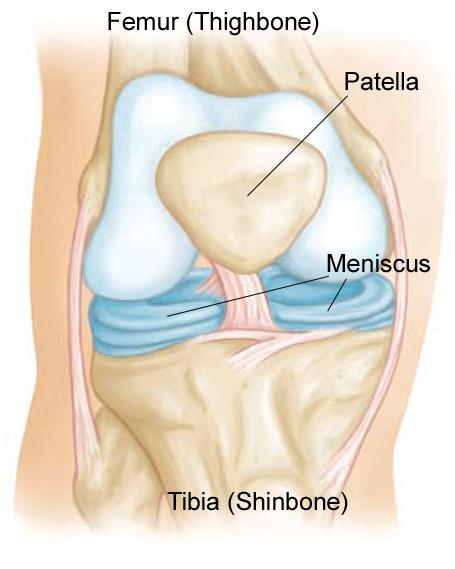
Two bones meet to form your knee joint: the femur and the tibia. The kneecap (patella) sits in front of the joint to provide some protection.
Two wedge-shaped pieces of fibrocartilage act as shock absorbers between your femur and tibia. These are the menisci. The menisci help to transmit weight from one bone to another and play an important role in knee stability.
Description
The meniscus can tear from acute trauma or as the result of degenerative changes that happen over time. Tears are noted by how they look, as well as where the tear occurs in the meniscus. Common tears include bucket handle, flap, and radial.
Sports-related meniscus injuries often occur along with other knee injuries, such as anterior cruciate ligament (ACL) tears.
Cause
Acute meniscus tears often happen during sports. These can occur through either a contact or non-contact injury — for example, a pivoting or cutting injury.
As people age, they are more likely to have degenerative meniscus tears. Aged, worn tissue is more prone to tears. An awkward twist when getting up from a chair may be enough to cause a tear in an aging meniscus.
Symptoms
You might feel a pop when you tear the meniscus. Most people can still walk on their injured knee, and many athletes are able to keep playing with a tear. Over 2 to 3 days, however, the knee will gradually become more stiff and swollen.
The most common symptoms of a meniscus tear are:
- Pain
- Stiffness and swelling
- Catching or locking of your knee
- The sensation of your knee giving way
- Inability to move your knee through its full range of motion
Doctor Examination
Physical Examination
After discussing your symptoms and medical history, your doctor will examine your knee. They will check for tenderness along the joint line where the meniscus sits. This often signals a tear.
One of the main tests for meniscus tears is the McMurray test. Your doctor will bend your knee, then straighten and rotate it. This puts tension on a torn meniscus. If you have a meniscus tear, this movement may cause pain, clicking, or a clunking sensation within the joint.
Imaging Tests
Because other knee injuries can cause similar symptoms, your doctor may order imaging tests to help confirm the diagnosis.
X-rays. X-rays provide images of dense structures, such as bone. Although an X-ray will not show a meniscus tear, your doctor may order one to look for other causes of knee pain, such as osteoarthritis.
Magnetic resonance imaging (MRI) scans. An MRI scan assesses the soft tissues in your knee joint, including the menisci, cartilage, tendons, and ligaments.
Treatment
The treatment your doctor recommends will depend on a number of factors, including your age, symptoms, and activity level. They will also consider the type, size, and location of the injury.
The outer one-third of the meniscus has a rich blood supply. A tear in this "red" zone may heal on its own, or can often be repaired with surgery. A longitudinal tear is an example of this kind of tear.
In contrast, the inner two-thirds of the meniscus lacks a significant blood supply. Without nutrients from blood, tears in this "white" zone with limited blood flow cannot heal. Because the pieces cannot grow back together, symptomatic tears in this zone that do not respond to conservative treatment are usually trimmed surgically.
Nonsurgical Treatment
Many meniscus tears will not need immediate surgery. If your symptoms do not persist and you have no locking or swelling of the knee, your doctor may recommend nonsurgical treatment.
RICE. The RICE protocol is effective for most sports-related injuries. RICE stands for Rest, Ice, Compression, and Elevation.
- Rest. Take a break from the activity that caused the injury. Your doctor may recommend that you use crutches to avoid putting weight on your leg.
- Ice. Use cold packs for 20 minutes at a time, several times a day. Do not apply ice directly to the skin.
- Compression. To prevent additional swelling and blood loss, wear an elastic compression bandage.
- Elevation. To reduce swelling, recline when you rest, and put your leg up higher than your heart.
Nonsteroidal anti-inflammatory drugs (NSAIDs). Anti-inflammatory drugs such as aspirin, ibuprofen, and naproxen help reduce pain and swelling.
Steroid injection. Your doctor may inject a corticosteroid medication into your knee joint to help eliminate pain and swelling.
Other nonsurgical treatment. Biologics injections, such as platelet-rich plasma (PRP), are currently being studied and may show promise in the future for the treatment of meniscus tears.
Surgical Treatment
If your symptoms persist with nonsurgical treatment, your doctor may suggest arthroscopic surgery.
Procedure. Knee arthroscopy is one of the most commonly performed surgical procedures. In this procedure, the surgeon inserts a miniature camera through a small incision (portal) in the knee. This provides a clear view of the inside of the knee. The surgeon then inserts surgical instruments through two or three other small portals to trim or repair the tear.
- Partial meniscectomy. In this procedure, the damaged meniscus tissue is trimmed away. This procedure typically allows for immediate weight bearing, and full range of motion soon after surgery.
- Meniscus repair. Some meniscus tears can be repaired by suturing (stitching) the torn pieces together. Whether a tear can be successfully repaired depends upon the type of tear, as well as the overall condition of the injured meniscus. Because the meniscus must heal back together, recovery time for a repair is longer than for a meniscectomy.
Once the initial healing is complete, your doctor will prescribe rehabilitation exercises. Regular exercise to restore your knee mobility and strength is necessary. You will start with exercises to improve your range of motion. Strengthening exercises will gradually be added to your rehabilitation plan.
In many cases, rehabilitation can be carried out at home, although your doctor may recommend working with a physical therapist. Rehabilitation time for a meniscus repair is about 3 to 6 months. A meniscectomy requires less time for healing — approximately 3 to 6 weeks.
Recovery
Meniscus tears are extremely common knee injuries. With proper diagnosis, treatment, and rehabilitation, patients often return to their pre-injury abilities.
Last Reviewed
March 2021
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.