Diseases & Conditions
Carpal Tunnel Syndrome
Carpal tunnel syndrome is a common condition that causes numbness, tingling, and pain in the hand and forearm. The condition occurs when one of the major nerves to the hand — the median nerve — is squeezed or compressed as it travels through the wrist.
In most patients, carpal tunnel syndrome gets worse over time. If untreated for too long, it can lead to permanent dysfunction of the hand, including loss of sensation in the fingers and weakness. For this reason, it is important to diagnose and treat carpal tunnel syndrome promptly.
Early symptoms can often be relieved with simple measures like:
- Wearing a wrist splint while sleeping
- Exercises to keep the nerve mobile
- Avoiding certain activities that aggravate your symptoms
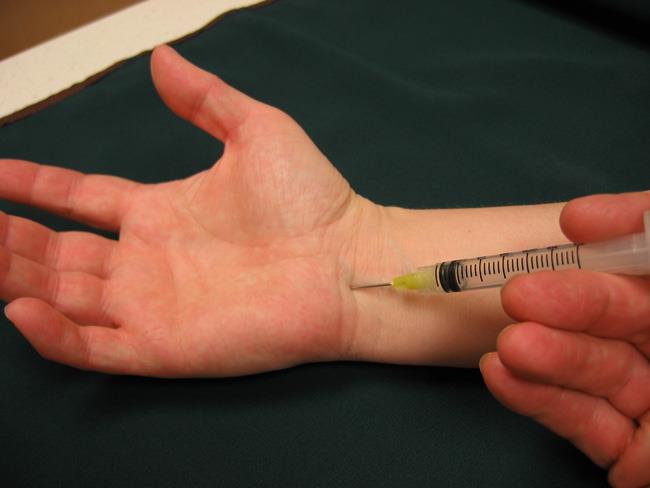
- A steroid injection into the carpal tunnel
If pressure on the median nerve continues, however, it can lead to nerve damage and worsening symptoms. To prevent permanent damage, surgery to take pressure off the median nerve may be recommended for some patients.
Anatomy
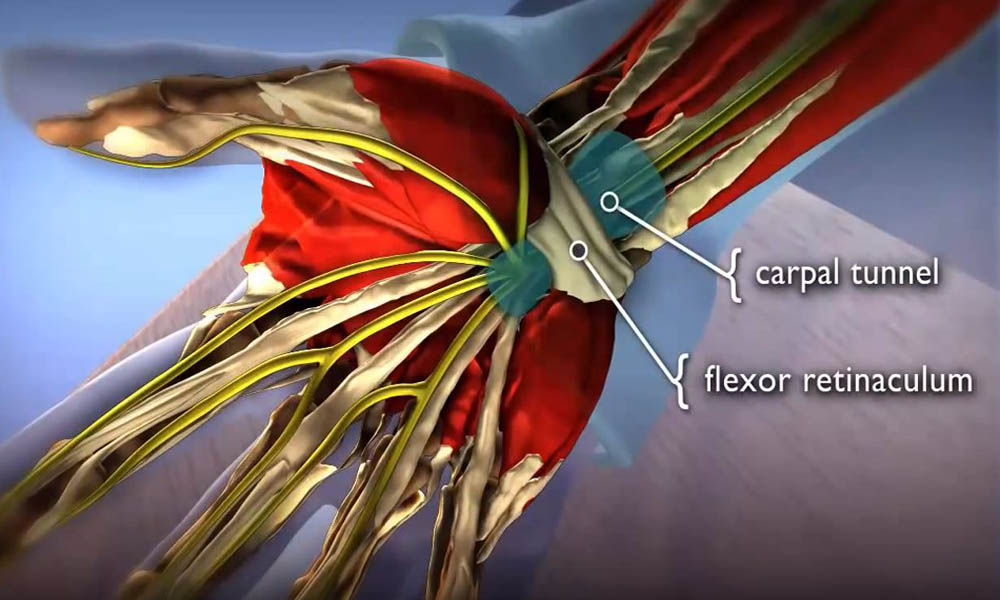
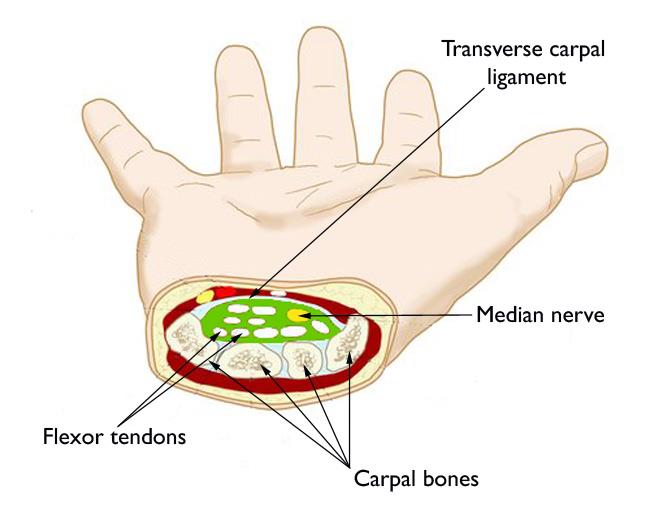
The carpal tunnel is a narrow passageway in the wrist, about an inch wide. The floor and sides of the tunnel are formed by small wrist bones called carpal bones.
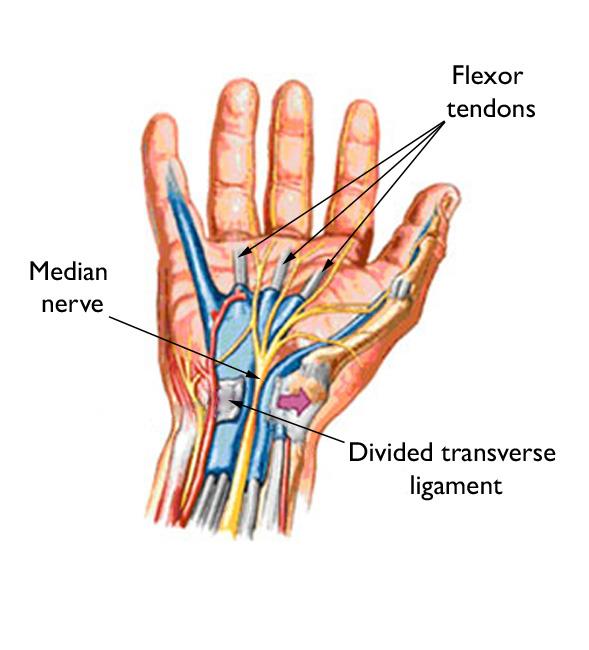
The roof of the tunnel is a strong band of connective tissue called the transverse carpal ligament. Because these boundaries are very rigid, the carpal tunnel has little capacity to stretch or increase in size.
The median nerve is one of the main nerves in the hand. It originates as a group of nerve roots in the neck; these roots then come together to form a single nerve in the arm.
The median nerve travels down the upper arm, across the elbow, and into the forearm, then passes through the carpal tunnel at the wrist on its way to the hand and fingers. It separates into several smaller nerves along the way, particularly once it reaches the palm. These nerves allow for feeling in the thumb, index finger, middle finger, and half of the ring finger (the thumb side).
The median nerve also controls the muscles around the base of the thumb.
The nine tendons that bend the fingers and thumb also travel through the carpal tunnel with the nerve. These tendons are called flexor tendons because they flex the fingers and thumb.
Description
Carpal tunnel syndrome occurs when the tunnel becomes narrowed or when the tissue surrounding the flexor tendons (known as synovium) swells, putting pressure on the median nerve and reducing its blood supply.
This abnormal pressure on the nerve can result in numbness, tingling, pain, and weakness in the hand.
Cause
Most cases of carpal tunnel syndrome are caused by a combination of factors. Studies show that women and older people are more likely to develop the condition.
Other risk factors for carpal tunnel syndrome include:
- Heredity. This is likely an important factor. The carpal tunnel may be naturally smaller in some people, or there may be anatomic differences that change the amount of space for the nerve — and these traits can run in families.
- Repetitive hand use. Repeating the same hand and wrist motions or activities over a prolonged period of time may aggravate the tendons in the wrist, causing swelling that puts pressure on the nerve.
- Hand and wrist position. Doing activities that involve extreme flexion or extension of the hand and wrist for a prolonged period of time can increase pressure on the nerve.
- Pregnancy. Hormonal changes during pregnancy can cause swelling that results in pressure on the nerve.
- Health conditions. Diabetes, rheumatoid arthritis, and thyroid gland imbalance are conditions that are associated with carpal tunnel syndrome.
Symptoms
Symptoms of carpal tunnel syndrome may include:
- Numbness, tingling, burning, and pain — primarily in the thumb and index, middle, and ring fingers. This often wakes people up at night.
- Occasional shock-like sensations that radiate to the thumb and index, middle, and ring fingers
- Pain or tingling that may travel up the forearm toward the shoulder
- Weakness and clumsiness in the hand — this may make it difficult to perform fine movements such as buttoning your clothes
- Dropping things — due to weakness, numbness, or a loss of proprioception (awareness of where your hand is in space)
In most cases, the symptoms of carpal tunnel syndrome begin gradually, without a specific injury. Many patients find that their symptoms come and go at first. However, as the condition worsens, symptoms may occur more frequently or may persist for longer periods of time.
Nighttime symptoms are very common. Because many people sleep with their wrists bent, symptoms may awaken you from sleep. During the day, symptoms often occur when holding something for a prolonged period of time with the wrist bent forward or backward, such as when using a phone, driving, or reading a book.
Many patients find that moving or shaking their hands helps relieve their symptoms.
Doctor Examination
Physical Examination
During your evaluation, your doctor will talk to you about your general health and medical history and will ask about your symptoms.
They will carefully examine your hand and wrist and perform a number of physical tests. During these tests, your doctor may:
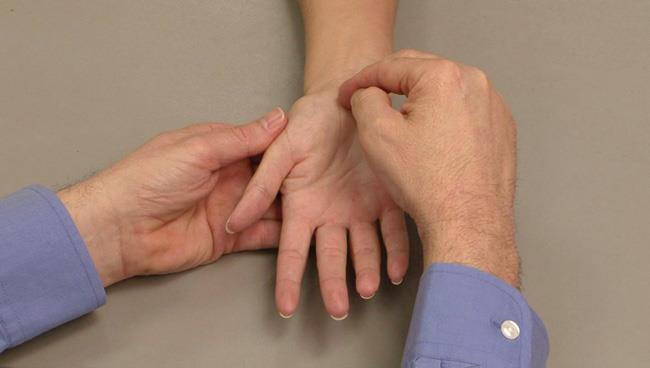
- Press down or tap along the median nerve on the palm side of your wrist and hand to see if it causes any tingling into your fingers (Tinel's sign).
- Bend and hold your wrists in a flexed position to test for numbness or tingling in your hands.
- Test sensitivity in your fingertips and hands by lightly touching them with a special instrument while your eyes are closed.
- Check for weakness in the muscles around the base of your thumb.
- Look for atrophy in the muscles around the base of your thumb. In severe cases, these muscles may become visibly smaller.
Tests
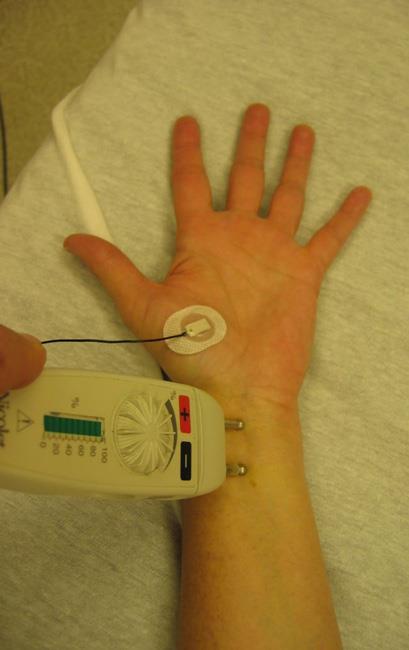
Electrophysiological tests. Your doctor may order electrophysiological testing of your nerves to measure how well your median nerve is working and help determine whether there is too much pressure on the nerve.
These tests will also help your doctor determine:
- The severity of your carpal tunnel syndrome
- Whether the nerve is compressed in other locations
- Whether other nerves are affected
- Whether you have a medical condition (e.g., neuropathy) affecting your nerves in addition to carpal tunnel syndrome
Electrophysiological tests may include:
- Nerve conduction studies (NCS). These tests measure the signals travelling in the nerves of your hand and arm and can detect when a nerve is not conducting its signal effectively. Nerve conduction studies can help your doctor determine how severe your problem is and help to guide treatment.
- Electromyogram (EMG). An EMG measures the electrical activity in muscles. EMG results can show whether you have any nerve or muscle damage.
Ultrasound. An ultrasound uses high-frequency sound waves to help create pictures of bone and tissue. Your doctor may recommend an ultrasound of your wrist to evaluate the median nerve for signs of compression.
X-rays. X-rays provide images of dense structures, such as bone. If you have limited wrist motion or wrist pain, your doctor may order X-rays to exclude other causes for your symptoms, such as arthritis, ligament injury, or a fracture.
Magnetic resonance imaging (MRI) scans. MRI scans provide better images of the body's soft tissues than X-rays. Your doctor may order an MRI to help determine other causes for your symptoms or to look for abnormal tissues that could be impacting the median nerve. An MRI can also help your doctor determine if there are problems with the nerve itself, such as a tumor or scarring from an injury.
Treatment
Although it is a gradual process, for most people carpal tunnel syndrome will worsen over time without some form of treatment. For this reason, it is important to be evaluated and diagnosed by your doctor early on. In the early stages, it may be possible to slow or stop the progression of the disease.
Nonsurgical Treatment
If diagnosed and treated early, the symptoms of carpal tunnel syndrome can often be relieved without surgery. If your diagnosis is uncertain or if your symptoms are mild, your doctor will recommend nonsurgical treatment first.
Nonsurgical treatments may include:
Bracing or splinting. Wearing a brace or splint at night will keep you from bending your wrist while you sleep. Keeping your wrist in a straight or neutral position reduces pressure on the nerve in the carpal tunnel. It may also help to wear a splint during the day when doing activities that aggravate your symptoms.
Nonsteroidal anti-inflammatory drugs (NSAIDs). Anti-inflammatory medications such as ibuprofen and naproxen can help relieve pain and inflammation.
Activity changes. Symptoms often occur when your hand and wrist are in the same position for too long — particularly when your wrist is flexed or extended.
If your job or recreational activities aggravate your symptoms, changing or modifying these activities can help slow or stop progression of the disease. In some cases, this may involve making changes to your work site or workstation.
Nerve gliding exercises. Some patients may benefit from exercises that help the median nerve move more freely within the confines of the carpal tunnel. Specific exercises may be recommended by your doctor or therapist.
Steroid injections. Corticosteroid, or cortisone, is a powerful anti-inflammatory agent that can be injected into the carpal tunnel. These injections often relieve painful symptoms or help to calm a flare-up of symptoms.
- In patients with mild, early disease, injections may relieve symptoms in the long-term.
- In those with moderate to severe disease, the positive effects of the injection may be temporary.
A cortisone injection may also be used by your doctor to help diagnose your carpal tunnel syndrome.
Surgical Treatment
If nonsurgical treatment does not relieve your symptoms or provides only temporary relief, your doctor may recommend surgery.
The decision of whether to recommend surgery is based on:
- The severity of your symptoms
- Physical exam findings
- Response to non-operative treatment
- Results of testing
In long-standing cases with constant numbness and wasting of your thumb muscles, surgery may be recommended to prevent irreversible damage. Surgery may also be recommended if you do not get relief with non-operative treatments and/or demonstrate significant nerve changes on testing.
Surgical Procedure
The surgical procedure performed for carpal tunnel syndrome is called a carpal tunnel release.
Most surgeons perform this procedure using one of two different surgical techniques, but the goal of both is to relieve pressure on your median nerve by cutting the ligament that forms the roof of the tunnel (transverse carpal ligament). Release of this ligament increases the size of the tunnel and decreases pressure on the median nerve, allowing for appropriate blood flow to the nerve and function of the nerve.
In most cases, carpal tunnel surgery is done on an outpatient basis. The surgery can be done under general anesthesia, which puts you to sleep, or under local anesthesia, which numbs just your hand and arm. In some cases where local anesthesia is used, you will also be given a light sedative through an intravenous (IV) line inserted into a vein in your arm.
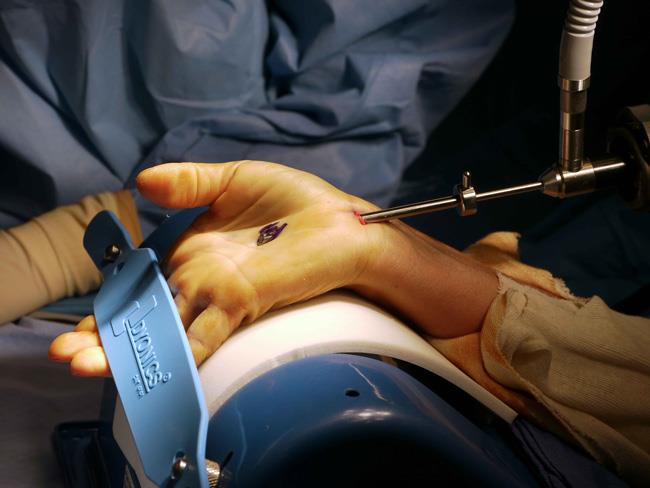
Open carpal tunnel release. In an open carpal tunnel release surgery, your doctor makes a small incision in the palm of your hand and views the inside of your hand and wrist through this incision. During the procedure, your doctor will divide the transverse carpal ligament (the roof of the carpal tunnel). This increases the size of the tunnel and decreases pressure on the median nerve.
After surgery, the ligament may gradually grow back together in a lengthened fashion, but there will be more space in the carpal tunnel, and pressure on the median nerve will be relieved.
Endoscopic carpal tunnel release. In endoscopic surgery, your doctor makes one or two smaller skin incisions (called portals) and uses a miniature camera, or endoscope, to see inside your hand and wrist. A special knife is used to divide the transverse carpal ligament, similar to the open carpal tunnel release procedure.
The outcomes of open surgery and endoscopic surgery are similar. There are benefits and potential risks associated with both techniques. Your doctor will talk with you about which surgical technique is best for you.
Recovery
Immediately after surgery, you will be encouraged to elevate your hand above your heart and move your fingers to reduce swelling and prevent stiffness.
You should expect some pain, swelling, and stiffness after your procedure. Minor soreness in your palm may last several weeks to several months.
Nighttime symptoms improve dramatically for most patients in the first week or so after surgery.
Grip and pinch strength
- Grip and pinch strength usually return by about 2 to 3 months after surgery.
- If the condition of your median nerve was poor before surgery, grip and pinch strength may not improve for about 6 to 12 months.
- In very severe cases, the normal strength you had before you developed carpal tunnel syndrome may not completely return. However, surgery is still important in these cases to prevent worsening of the condition and function of your nerve.
Numbness and tingling
- Numbness and tingling tend to improve over the first several months after surgery.
- Some patients with mild disease may experience return of sensation right away.
- Patients with severe disease may not have normal sensation in their fingertips for 6 to 12 months after surgery.
- In very severe cases, some patients may never completely regain normal sensation. Again, surgery is still important in these cases to prevent the condition from getting worse.
You may have to wear a splint or wrist brace for several weeks after surgery. You will be allowed to use your hand for light activities, taking care to avoid significant discomfort. Driving, self-care activities, and light lifting and gripping may be permitted soon after surgery.
Your doctor will talk with you about when you will be able to return to work and whether you will have any restrictions on your work activities.
Complications
Although complications are possible with any surgery, your doctor and surgical team will take steps to minimize the risks. The most common complications of carpal tunnel release surgery include:
- Bleeding
- Infection
- Wound healing issues
- Nerve aggravation or injury
Outcomes
For most patients, surgery will improve the symptoms of carpal tunnel syndrome. Recovery, however, may be gradual, and complete recovery may take up to a year.
If you have significant pain and weakness for more than 2 months, your doctor may refer you to a hand therapist who can help you maximize your recovery.
If you have another condition that causes pain or stiffness in your hand or wrist, such as arthritis or tendinitis, it may slow your overall recovery. In long-standing cases of carpal tunnel syndrome with severe loss of feeling and/or muscle wasting around the base of the thumb, recovery will also be slower. For these patients, a complete recovery may not be possible.
Occasionally, carpal tunnel syndrome can recur, although this is rare. If this happens, you may need additional treatment or surgery.
To assist doctors in the management of carpal tunnel syndrome, the American Academy of Orthopaedic Surgeons has conducted research to provide some useful guidelines. These are recommendations only and may not apply to every case. For more information: Plain Language Summary - Clinical Practice Guideline - Carpal Tunnel Syndrome - AAOS
Last Reviewed
March 2022
Contributed and/or Updated by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.