Treatment
ACL Injury: Does It Require Surgery?
The following article provides in-depth information about treatment for anterior cruciate ligament injuries. It does not discuss knee anatomy, or the causes, symptoms, and diagnosis of ACL injuries. The article Anterior Cruciate Ligament (ACL) Injuries covers these topics and is recommended reading prior to this article.
The information that follows includes treatment options for ACL injuries along with a description of ACL surgical techniques and rehabilitation, potential complications, and outcomes.
This information is intended to assist the patient in making the best-informed decision possible regarding the management of ACL injury.
Description
The ACL is one of the most commonly injured ligaments of the knee.
Approximately half of ACL injuries occur along with damage to the meniscus, articular cartilage, or other ligaments.
Injured ligaments are considered sprains and are graded on a severity scale.
Grade 1 Sprains. The ligament is mildly damaged in a Grade 1 sprain. It has been slightly stretched but is still able to help keep the knee joint stable.
Grade 2 Sprains. A Grade 2 sprain stretches the ligament to the point where it becomes loose. This is often referred to as a partial tear of the ligament.
Grade 3 Sprains. This type of sprain is most commonly referred to as a complete tear of the ligament. The ligament has been torn in half or pulled directly off the bone, and the knee joint is unstable.
Partial tears of the anterior cruciate ligament are rare; most ACL injuries are complete or near complete tears.
What happens naturally with an ACL injury without surgery varies from patient to patient and depends on the patient's activity level, degree of injury, and instability symptoms.
Partial ACL Tears
The prognosis (outlook) for a partially torn ACL is often good, with the recovery and rehabilitation period usually lasting at least 3 months.
However, some patients with partial ACL tears may still have instability symptoms. Close clinical follow-up and a complete course of physical therapy help identify those patients with unstable knees due to partial ACL tears.
Complete ACL Tears
Complete ACL tears have a much less positive outcome without surgery.
After a complete ACL tear, some patients are unable to participate in cutting- or pivoting-type sports, while others have instability during even normal activities, such as walking. There are some rare individuals who can participate in sports without any symptoms of instability. This variability is related to the severity of the original knee injury, as well as the physical demands of the patient.
About half of ACL injuries occur in combination with damage to the meniscus, articular cartilage (the smooth cartilage that covers the ends of bones), or other ligaments.
Secondary (related) damage may occur in patients who have repeated episodes of instability due to ACL injury. With chronic instability, the majority of patients will have meniscus damage 10 or more years after the initial injury. Similarly, articular cartilage lesions are more common in patients who have a 10-year-old ACL deficiency.
Nonsurgical Treatment
Progressive physical therapy and rehabilitation can restore the knee to a condition close to its pre-injury state and teach the patient how to prevent instability. The doctor may also recommend wearing a hinged knee brace for added support. However, many people who choose not to have surgery suffer an injury to another part of the knee due to instability in the joint.
Surgical treatment is usually recommended for combined injuries (ACL tears that occur along with other injuries in the knee). However, deciding against surgery is reasonable for certain patients.
Nonsurgical management of isolated ACL tears is likely to be successful or may be recommended in patients:
- With partial tears and no instability symptoms
- With complete tears who don't experience symptoms of knee instability during low-demand sports and are willing to give up high-demand sports
- Who do light manual work or live sedentary (inactive) lifestyles
There is increasing evidence that children with ACL tears are at high risk for future damage to the meniscus or cartilage with nonsurgical management. If your child or adolescent has open growth plates and an ACL tear, talk to the surgeon about the risks and benefits of surgery, as the growth plates can be avoided with certain surgical techniques.
Surgical Treatment
ACL tears are not usually repaired using sutures (stitches) because repaired ACLs have generally been shown to fail over time.
Recent studies have focused on the repair of certain types of ACL tears (typically, an avulsion, or separation, of the ligament from where it attaches to the femur, or thighbone) with various techniques and the potential use of biologics to promote healing; however, long-term studies do not yet support widespread use.
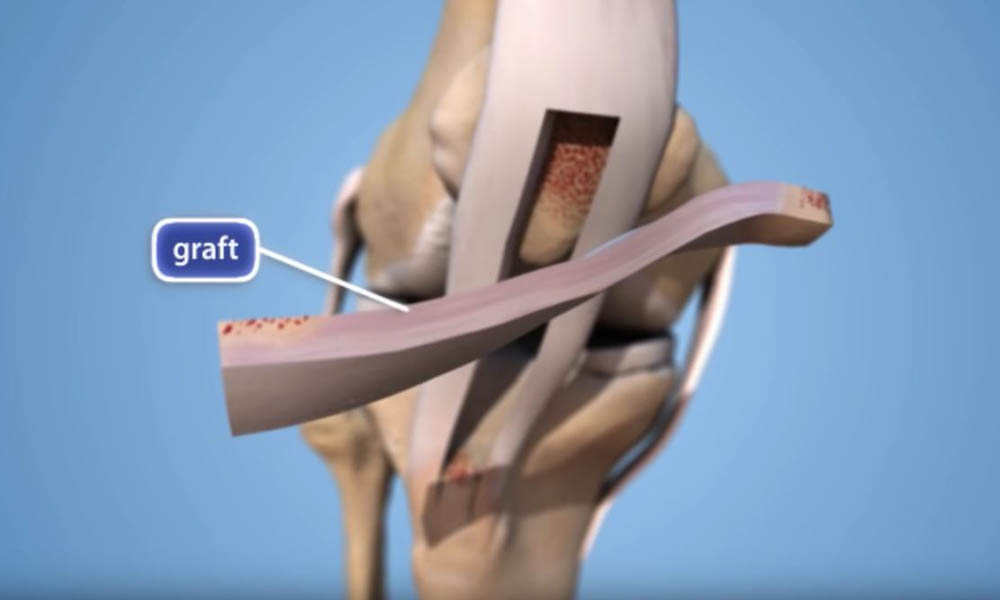
Therefore, the torn ACL is generally replaced by a substitute graft made of tendon, including:
- Patellar, hamstring, or quadriceps tendon autograft (autografts come from the patient)
- Patellar tendon, Achilles tendon, semitendinosus, gracilis, or posterior tibialis tendon allograft (allografts come from a tissue donor)
Who Should Consider ACL Reconstruction Surgery?
- Active adult patients who are involved in sports or jobs that require pivoting, turning, or hard-cutting, or who perform heavy manual work are encouraged to consider surgical treatment. This includes older patients who have previously been excluded from consideration for ACL surgery. Activity level, not age, should determine whether surgery should be considered.
- In young children or adolescents with ACL tears, early ACL reconstruction creates a possible risk of growth plate injury, leading to bone growth problems. However, recent studies support early ACL reconstruction, as delaying treatment can lead to a higher rate of future meniscus or cartilage injuries.
- A patient with a torn ACL and significant functional instability has a high risk of developing damage in other areas of the knee and should therefore consider ACL reconstruction.
- It is common to see ACL injuries combined with damage to the menisci, articular cartilage, collateral ligaments, joint capsule, or a combination of the above. The "unhappy triad," frequently seen in football players and skiers, consists of injuries to the ACL, the MCL, and the medial meniscus. In cases of combined injuries, surgical treatment may be necessary and generally produces better outcomes. As many as half of meniscus tears may be fixable, and they may heal better if the repair is done at the same time as the ACL reconstruction.
Surgical Options
Patellar tendon autograft. A patellar tendon autograft is made up of the middle third of the patient's patellar tendon, along with a bone plug from the shin and the kneecap. Considered by some surgeons as the "gold standard" graft for ACL reconstruction, it is often recommended for high-demand athletes and patients whose jobs do not require a significant amount of kneeling.
In studies comparing outcomes of patellar tendon and hamstring autograft ACL reconstruction, the rate of graft failure was lower in the patellar tendon group. In addition, most studies show equal or better outcomes in terms of post-operative tests for knee laxity, or looseness, when this graft is compared to others.
The potential drawbacks of the patellar tendon autograft are:
- Post-operative pain behind the kneecap
- Pain with kneeling
- Slightly increased risk of post-operative stiffness
- Slight risk of patellar (kneecap) fracture
Hamstring tendon autograft. The hamstring tendon autograft uses the semitendinosus hamstring tendon on the inner side of the knee. Some surgeons use an additional tendon, the gracilis, which is attached below the knee in the same area. This creates a two- or four-strand tendon graft. Hamstring graft supporters claim there are fewer problems associated with harvesting the graft compared to the patellar tendon autograft, including:
- Less anterior (kneecap) knee pain after surgery
- Less postoperative stiffness
- Smaller incision
- Faster recovery
However, there may be drawbacks to using a hamstring graft, including:
- Post-operative function may be more limited than with the patellar tendon graft.
- The grafts may be slightly more vulnerable to stretching, which can lead to increased laxity (looseness) in the knee.
- The patient may have decreased hamstring strength after surgery.
Quadriceps tendon autograft. The quadriceps tendon autograft is often used for primary (initial) reconstruction as well as revision (repeat) reconstruction procedures. The surgeon uses the middle third of the patient's quadriceps tendon and a bone plug from the upper end of the kneecap, which produces a larger graft for taller and heavier patients.
Potential drawbacks include the following:
- Because there is a bone plug on one side only, the fixation is not as solid as for the patellar tendon graft, so loosening may occur.
- There is a high association with post-operative pain in front of the knee and a slight risk of patella fracture.
- Patients may find the incision is not cosmetically appealing.
Allografts. Grafts taken from human donors are safe, effective choices for certain patients. Allografts are also used for patients who have failed ACL reconstruction before and during surgery to repair or reconstruct more than one knee ligament.
Advantages of using allograft tissue include:
- Elimination of pain caused by obtaining the graft from the patient
- Decreased surgery time
- Smaller incisions
With modern sterilization techniques, the risk of any form of disease transmission from donor to recipient is exceptionally low.
Some studies, however, may point to a higher failure rate with the use of allografts for ACL reconstruction. Higher failure rates for allografts have been reported in young, active patients returning to high-demand sporting activities after ACL reconstruction, compared with autografts.
The reason for this higher failure rate is unclear. It could be due to graft material properties (sterilization processes used, graft donor age, storage of the graft). It could also be because the athletes thought the allograft would enable a faster recovery and returned to their sports too soon — before the graft was ready to withstand the loads and stresses of sports. More research is needed to determine whether allografts are a good option for this patient population.
Surgical Procedure
Before any surgical treatment, the patient is often sent to physical therapy. Patients who have a stiff, swollen knee lacking full range of motion at the time of ACL surgery may have significant problems regaining motion after surgery. It may take several weeks from the time of injury for the swelling and stiffness to subside enough to proceed with surgery.
Additionally, it is sometimes recommended that ligaments injured at the same time as the ACL be braced and allowed to heal before ACL surgery. For example, medial collateral ligament (MCL) injuries that occur along with ACL injuries often heal without surgery, so it's possible that only the ACL would need to be addressed during the surgery.
The patient, the surgeon, and the anesthesiologist will select the anesthesia used for surgery. Patients may benefit from an anesthetic block of the nerves of the leg to decrease post-operative pain.
The surgery usually begins with an examination of the patient's knee while the patient is relaxed (after being given anesthesia). This final examination is used to verify that the ACL is torn and to check for looseness of other knee ligaments that may need to be repaired during surgery or addressed post-operatively.
If the physical exam strongly suggests the ACL is torn, the surgeon will prepare the graft. They either harvest (for an autograft) or thaw (for an allograft) the selected tendon and create the graft to the correct size for the patient.
After the graft has been prepared, the surgeon makes small (1cm) incisions called portals in the front of the knee and inserts the arthroscope and instruments.
Once the arthroscope and instruments are in place, the surgeon will examine the condition of the knee, trim or repair any meniscus and cartilage injuries, and then remove the torn ACL stump.
In the most common ACL reconstruction technique, the surgeon drills bone tunnels into the tibia and the femur so they can place the ACL graft in a way that is as anatomically correct as possible. Once the graft is placed into the knee, it is held under tension and fixed in place with screws, buttons, or other device. These devices are generally not removed after surgery.
The surgeon then closes the skin incisions and applies dressings over them. The surgeon may also put a post-operative brace and cold therapy device on the patient's knee. The patient will usually go home the same day as their surgery.
Pain Management
After surgery, you will feel some pain. This is a natural part of the healing process. Your doctor and nurses will work to reduce your pain.
Medications are often prescribed for short-term pain relief after surgery. Many types of medicines are available to help manage pain, including opioids, non-steroidal anti-inflammatory drugs (NSAIDs), and local anesthetics. Your doctor may use a combination of these medications to improve pain relief, as well as minimize the need for opioids.
Be aware that although opioids help relieve pain after surgery, they are a narcotic and can be addictive. Opioid dependency and overdose have become critical public health issues in the U.S. It is important to use opioids only as directed by your doctor and to stop taking them as soon as your pain begins to improve. Talk to your doctor if your pain has not begun to improve within a few days of your surgery.
Rehabilitation
Physical therapy is a crucial part of successful ACL surgery, with exercises beginning immediately after the surgery. Much of the success of ACL reconstructive surgery depends on the patient's dedication to rigorous physical therapy. With new surgical techniques and stronger graft fixation, current physical therapy uses an accelerated course of rehabilitation.
Post-operative Course. In the first 7 to 10 days after surgery, the wound is kept clean and dry, and early emphasis is placed on regaining the ability to fully straighten the knee and restore quadriceps control.
The knee is iced regularly to reduce swelling and pain. The surgeon may order the use of a post-operative brace and a machine to move the knee through its range of motion, although this machine has not been shown to significantly improve patient outcomes.
Weightbearing status (use of crutches to keep some or all of the patient's weight off of the surgical leg) is also determined by physician preference, as well as other injuries addressed at the time of surgery.
Rehabilitation. The goals for rehabilitation of ACL reconstruction include:
- Reducing knee swelling
Maintaining mobility of the kneecap to prevent anterior knee pain problems or stiffness - Regaining full range of motion of the knee
- Strengthening the quadriceps and hamstring muscles
The patient may return to sports when:
- There is no longer pain or swelling
- They have achieved full range of motion in the knee
- Muscle strength, endurance, and functional use of the leg are fully restored
- Sense of balance and control of the leg are fully restored (through exercises designed to improve neuromuscular control).
Most patients are allowed to return to full sports participation within 6 to 12 months, depending on the patient's progress, strength, and mechanics.
The use of a functional brace when returning to sports is not necessarily required after a successful ACL reconstruction, but some patients may feel a greater sense of security by wearing one.
Potential Surgical Complications
Infection. The risk of infection after arthroscopic ACL reconstruction is very low. There have also been reported deaths linked to bacterial infection from allograft tissue due to improper procurement and sterilization techniques.
Viral transmission. Allografts specifically are associated with risk of viral transmission, including HIV and Hepatitis C, despite careful screening and processing. The chance of obtaining a bone allograft from an HIV-infected donor is calculated to be less than 1 in 1 million.
Bleeding, numbness. Rare risks include bleeding from acute injury to the popliteal artery, and weakness or paralysis of the leg or foot. It is not uncommon to have numbness of the outer part of the upper leg next to the incision, which may be temporary or permanent.
Blood clot. Although rare, a blood clot in the veins of the calf or thigh is a potentially life-threatening complication. A blood clot may break off in the bloodstream and travel to the lungs, causing pulmonary embolism or to the brain, causing stroke.
Instability. Chronic instability due to rupture or stretching of the reconstructed ligament or poor surgical technique is possible. It occurs in 5 to 10% of patients, long-term.
Stiffness. Knee stiffness or loss of motion has been reported by some patients after surgery and sometimes needs to be addressed surgically. The surgeon will either resect (remove) scar tissue or manipulate the knee under anesthesia.
Extensor mechanism failure. Rupture of the patellar tendon (patellar tendon autograft) or patella fracture (patellar tendon or quadriceps tendon autografts) may occur due to weakening at the site where the graft was harvested (removed).
Growth plate injury. In young children or adolescents with ACL tears, early ACL reconstruction creates a possible risk of growth plate injury, leading to bone growth problems. ACL surgery can be delayed until the child is closer to reaching skeletal maturity; however, this comes with a risk of future meniscus or cartilage injury. Alternatively, the surgeon may be able to modify the ACL reconstruction technique to decrease the risk of growth plate injury during surgery.
Kneecap pain. Post-operative anterior (front of the) knee pain is especially common after patellar tendon autograft ACL reconstruction. The incidence of pain behind the kneecap varies greatly in studies, whereas the incidence of kneeling pain is often higher after patellar tendon autograft ACL reconstruction.
To assist doctors in the management of anterior cruciate (ACL) ligament injuries, the American Academy of Orthopaedic Surgeons has conducted research to provide some useful guidelines. These are recommendations only and may not apply to every case. For more information: Plain Language Summary - Clinical Practice Guideline - Anterior Cruciate Ligament Injury - AAOS
Last Reviewed
October 2022
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.